Blue Light Effects on Eyes and Sleep | G2
What Is Blue Light, Really?
When scientists discuss blue light, they refer to a specific slice of the electromagnetic spectrum: the visible light region spanning roughly 400 to 500 nanometers [1]. This places blue light directly between ultraviolet radiation (which cuts off around 400 nm) and the longer visible wavelengths we perceive as green, yellow, and red.
From a physics perspective, energy distinguishes blue light from other colors. A photon’s energy follows a fundamental rule: it increases as its wavelength decreases. Because blue light sits at the shorter end of the visible spectrum, its photons carry more energy than those of any other color we can see.
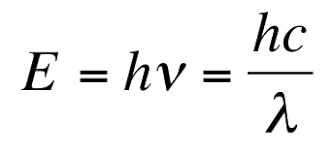
This fundamental physics means blue light photons carry more energy than those of any other color we can see. This higher energy forms the physical basis for both the benefits and the potential risks of blue light exposure; a duality that continues to spark considerable scientific interest and public debate.
However, popular media often misses a crucial point: blue light is not a modern invention. The sun has always been humanity’s most powerful source of blue light. What has changed in recent decades, rather, is our exposure patterns. Both the timing of our light exposure and its sources have shifted dramatically [2].
The Physics of Light and the Eye
To understand how blue light affects us, we must trace its journey through the eye. Our eyes function as sophisticated optical instruments, designed to focus light onto the retina; a specialized layer of photoreceptor cells. However, not all wavelengths reach this destination equally.
The cornea and crystalline lens act as natural filters along this path. The lens, notably, transforms throughout our lives. It gradually yellows with age, absorbing an increasing proportion of short-wavelength light [3]. This explains why infants and children experience much greater blue light transmission to their retinas than older adults; a fact with profound implications for understanding both visual development and age-related eye conditions.
Then, in 1998, researchers made a discovery that revolutionized our understanding of light’s biological effects [4]. They identified a new type of photoreceptor in the eye. Unlike the rods and cones responsible for vision, these intrinsically photosensitive retinal ganglion cells (ipRGCs) serve a completely different purpose: they detect ambient light levels and communicate directly with the brain’s master clock; the suprachiasmatic nucleus [5].
These ipRGCs contain a photopigment called melanopsin, which reaches peak sensitivity at approximately 479 nm; right in the blue portion of the spectrum [6]. This provides the physical basis for blue light’s powerful influence on our circadian rhythms, a topic we will explore in detail.
The Circadian Connection: How Light Sets Our Internal Clock
The human body operates on roughly 24-hour cycles called circadian rhythms. These rhythms govern far more than just when we sleep and wake. They also regulate hormone secretion, body temperature, metabolism, and even cognitive performance [7].
At the helm of this system sits the suprachiasmatic nucleus (SCN) in the hypothalamus, serving as our master clock. It coordinates these rhythms throughout the body, but it cannot do so alone. The SCN needs external cues – zeitgebers, in chronobiology terminology – to stay synchronized with the outside world. And among these cues, light proves most powerful.
Here’s what happens when blue light strikes the ipRGCs: melanopsin undergoes a photochemical change, triggering a signal cascade. This signal then travels via the retinohypothalamic tract to the SCN, which in turn influences the pineal gland’s production of melatonin; the hormone that facilitates sleep [8].
This brings us to a crucial physics-biology connection: the spectral sensitivity of this system peaks in the blue range. Consequently, blue light suppresses melatonin far more effectively than longer wavelengths. Studies demonstrate that exposure to 460 nm light suppresses melatonin for roughly twice as long as exposure to 555 nm light (the peak sensitivity of our visual system), even when researchers match photon density between the two conditions [9].
This is no design flaw, it is an evolutionary adaptation. Sunlight floods our environment with blue light during daytime, signaling our bodies to stay wakeful and alert. Then, as the sun sets, the spectral composition shifts toward longer wavelengths. This shift allows melatonin to rise naturally, preparing our bodies for restful sleep.
The Day-Night Duality: When Blue Light Helps and When It Harms
The effects of blue light depend critically on timing; a concept that physics alone cannot capture but that physiology makes clear.
Daytime Benefits
During daylight hours, blue light exposure serves several important functions:-
- Alertness and cognitive function: Blue light actively stimulates brain regions involved in attention and cognitive performance. Studies consistently show that daytime blue light exposure improves reaction times and reduces subjective sleepiness [10].
- Mood regulation: Blue light influences serotonin production, therefore, contributing to mood stability and well-being.
- Circadian synchronization: Proper daytime blue light exposure ensures that the internal clock remains aligned with the external day-night cycle, hence, promoting consolidated sleep at night.

Evening Concerns
The problem arises when blue light exposure occurs in the evening; the time when the body expects diminishing light and prepares for sleep. Evening blue light exposure can:-
- Suppress melatonin: Even relatively dim blue light can significantly reduce melatonin production [11].
- Delay circadian timing: Light exposure in the hours before bedtime can phase-shift the circadian clock, making it harder to fall asleep at the desired time.
- Increase alertness: The same alerting effects that are beneficial during the day become problematic at night, interfering with sleep initiation [12].
A systematic review by Silvani et al. (2022) examining blue light’s influence on sleep reveals an intriguing pattern. Approximately half of the studies reviewed reported decreased tiredness with blue light exposure. Yet about one-third found decreased sleep duration, and half observed decreased sleep efficacy [13].
This apparent contradiction resolves neatly when we consider timing. Daytime exposure reduces tiredness; a clear benefit. Evening exposure, by contrast, can compromise sleep quality and duration; a definite drawback.

The Digital Device Question: Are Screens the Problem?
The widespread adoption of LED-backlit screens has intensified public concern about blue light exposure. White LEDs, the technology powering most modern displays, emit light with a distinct spectral peak in the blue region, typically around 450-460 nm [14]. This peak coincides closely with both the circadian sensitivity maximum 479 nm and the so-called blue light hazard function (approximately 440 nm).
However, intensity matters and this is where physics offers important perspective. Digital devices emit blue light at levels orders of magnitude lower than natural daylight. Studies measuring the blue light hazard from electronic displays confirm that even prolonged viewing falls well below international exposure limits [15].
This brings us to a crucial distinction: the concern about evening screen use centers primarily on circadian disruption, not retinal damage. The former occurs at relatively low light levels. The latter, by contrast, requires intensities far higher than any screen produces.

The Cataract Surgery Connection: A Natural Experiment
Some of the most elegant evidence for blue light’s role in sleep regulation comes from an unexpected source: cataract patients. As the natural lens clouds with age, it reduces transmission of all light. However, short wavelengths suffer the most due to progressive yellowing. Fortunately, cataract surgery replaces this aged lens with an artificial intraocular lens (IOL), effectively resetting the eye’s optical properties.
During this procedure, patients can receive one of two common IOL types: conventional ultraviolet-filtering IOLs (UVF-IOLs) or blue-light-filtering IOLs (BF-IOLs) that also block some visible blue light. This clinical choice, therefore, creates a natural experiment for studying how blue light affects sleep.
A 2021 meta-analysis by Lee and colleagues compared these two IOL types. Intriguingly, they found weak evidence that UVF-IOLs – which transmit more blue light – produced greater improvement in subjective sleep quality than BF-IOLs at 3-8 weeks after surgery. Notably, however, this difference disappeared by 7-12 months [16]. The authors suggest this pattern may reflect the circadian system adapting to its new light environment: an initial response to acute change, followed by gradual habituation.
Here’s what makes this finding particularly compelling: cataract surgery increases blue light transmission by approximately 250% with BF-IOLs and 300% with UVF-IOLs [17]. As a result, this dramatic increase helps explain why so many older adults report improved sleep after surgery. In essence, they are suddenly receiving far more circadian-effective light during daytime hours.
The Retinal Damage Question: Separating Physics from Physiology
Perhaps the most controversial aspect of the blue light discussion concerns potential retinal damage. The physical basis for this concern comes from in vitro and animal studies demonstrating that short-wavelength light can induce photochemical damage in retinal pigment epithelial cells through the generation of reactive oxygen species (ROS) [18].
Here’s how this mechanism works: chromophores in the retina – particularly lipofuscin, which accumulates as we age – absorb blue light. This absorption can then trigger oxidative stress and cellular damage [19].
However, we must exercise caution when extrapolating from these laboratory conditions to real-world human exposure. Several physical factors demand careful attention:-
- Intensity: Laboratory studies use light intensities far exceeding typical environmental exposure.
- Duration: The relationship between exposure duration and damage is complex, with thresholds below which protective mechanisms can cope.
- Spectral composition: The action spectrum for retinal damage peaks around 440 nm, but environmental light sources have varying spectral distributions.
A comprehensive review by Zhao et al. (2018) notes an important caveat: while blue light between 415-455 nm can cause photochemical retinal damage in experimental settings, whether this translates to human pathology remains actively debated [20]. Consequently, the authors emphasize that normal digital displays present minimal risks for short-term exposure. Nevertheless, they advise caution regarding long-term cumulative exposure, as the evidence here remains less certain.
A 2017 systematic review by Lawrenson and colleagues adds another crucial piece to this puzzle. Specifically, they found no high-quality clinical trial evidence supporting blue-blocking spectacle lenses for macular protection in the general population [21].
At this point, we must be clear about what this finding means, and just as importantly, what it does not. First and foremost, this does not imply that blue light poses no risk whatsoever. Rather, it suggests that under normal environmental exposure, the risk appears low enough that protective eyewear has not demonstrated measurable benefits in clinical studies to date. Furthermore, this conclusion applies specifically to the general population; individuals with certain eye conditions or exceptional light exposure might still benefit, though research has yet to confirm this.
Blue-Blocking Lenses: What Does the Evidence Show?
Given the theoretical concerns surrounding blue light, researchers and manufacturers have developed various interventions to reduce exposure. Among these, blue-blocking spectacle lenses, which filter short-wavelength light, have become widely marketed for improving sleep and reducing eye strain.
Fortunately, we do not have to rely on marketing claims alone. A rigorous 2023 Cochrane systematic review by Singh and colleagues evaluated 17 randomized controlled trials comparing blue-blocking lenses with non-blue-blocking lenses [22]. Their findings offer valuable clarity, and they break down as follows:-
- Visual fatigue: There was no significant difference in subjective visual fatigue scores between blue-blocking and control lenses.
- Sleep quality: Evidence was inconsistent, with three studies showing improvement and three showing no effect. The authors rated the certainty of evidence as very low due to heterogeneous study populations and methodological limitations.
- Macular health: No studies evaluated effects on macular structure or function.
- Adverse effects: Reported adverse events were mild and included headache, discomfort, and mood changes; similar to those reported with control lenses.
Building on this evidence, another systematic review by Shechter et al. (2020) focused specifically on sleep outcomes. Their analysis revealed small-to-moderate combined effect sizes for objective sleep efficiency and total sleep time. Importantly, they observed larger effects in individuals with sleep or psychiatric disorders compared to healthy participants [23].
This pattern points to a crucial takeaway: blue-blocking interventions may offer the greatest benefit for vulnerable populations. Specifically, people with insomnia, bipolar disorder, or delayed sleep phase syndrome appear most likely to experience improvements. For healthy good sleepers, by contrast, the benefits appear limited at best.
Practical Implications: Timing Matters More Than Blocking
The physics and physiology reviewed above converge on a practical message: timing of light exposure matters more than absolute avoidance of blue light.
Daytime Recommendations
- Seek bright light exposure, particularly in the morning, to reinforce circadian synchronization.
- Natural daylight remains the best source; it’s intense, spectrally rich, and free.
- If you work indoors, consider sitting near windows or using bright, blue-enriched lighting during work hours.
Evening Recommendations
- Reduce exposure to bright light, particularly from screens, in the 2-3 hours before bedtime.
- Use device features that shift display color temperature toward warmer tones in the evening; these reduce blue light emission while maintaining usability.
- If you’re particularly sensitive to evening light or have sleep difficulties, amber-tinted glasses that filter blue light may be helpful. These are most effective when worn consistently before bedtime [24].
Special Populations
- Older individuals: Age-related lens yellowing reduces blue light transmission. Ensuring adequate daytime blue light exposure – or considering the spectral characteristics of indoor lighting – may help maintain circadian function [25].
- People with sleep disorders: Blue-blocking interventions appear more promising for those with established sleep difficulties, particularly when combined with other sleep hygiene measures.
- Children and adolescents: Their clearer lenses transmit more blue light to the retina, and their evening device use is often high. Evening screen-time limits and blue-reducing settings are reasonable precautions.
Conclusion: A Balanced Perspective
Let us be clear from the outset: blue light is not inherently harmful. On the contrary, it serves as an essential environmental signal that has shaped human biology for millennia. The very same physical properties that give blue light its higher energy also make it the most effective signal for synchronizing our internal clocks with the world outside.
The modern concern about blue light, therefore, reflects a fundamental mismatch between our evolutionary heritage and our current environment. We have, after all, created light sources that allow us to remain active at any hour. Yet our circadian systems still expect the ancient pattern: bright days and dark nights.
Synthesizing the evidence reviewed here, a nuanced conclusion emerges:
- Daytime blue light is beneficial for alertness, mood, and circadian health.
- Evening blue light can be problematic for sleep, particularly when exposure occurs close to bedtime.
- The risk of retinal damage from normal device use appears low, based on current evidence.
- Blue-blocking interventions show promise for specific populations but are not universally necessary.
The physics of blue light is straightforward; its biological effects are complex and context-dependent. Understanding both allows us to make informed decisions about our light environment; not from fear, but from knowledge of how light shapes our days and nights.
References
[1] Edem GD, David JU, Amadi MA, Nwajah SD. The Impact of Blue Light on Eye Health- A Brief Review. Clinical Research and Clinical Reports. 2024;3(12). DOI:10.31579/2835-8325/1100
[2] Wahl S, Engelhardt M, Schaupp P, Lappe C, Ivanov IV. The inner clock: Blue light sets the human rhythm. Journal of Biophotonics. 2019;12:e201900102.
[3] Zhao ZC, Zhou Y, Tan G, Li J. Research progress about the effect and prevention of blue light on eyes. International Journal of Ophthalmology. 2018;11(12):1999-2003.
[4] Provencio I, Jiang G, Willem J, Hayes WP, Rollag MD. Melanopsin: An opsin in melanophores, brain, and eye. Proceedings of the National Academy of Sciences. 1998;95(1):340-345.
[5] Berson DM, Dunn FA, Takao M. Phototransduction by retinal ganglion cells that set the circadian clock. Science. 2002;295(5557):1070-1073.
[6] Bailes HJ, Lucas RJ. Human melanopsin forms a pigment maximally sensitive to blue light supporting activation of G(q/11) and G(i/o) signalling cascades. Proceedings of the Royal Society B. 2013;280:20122987.
[7] Dijk DJ, Lockley SW. Integration of human sleep-wake regulation and circadian rhythmicity. Journal of Applied Physiology. 2002;92(2):852-862.
[8] Gooley JJ, Lu J, Chou TC, Scammell TE, Saper CB. Melanopsin in cells of origin of the retinohypothalamic tract. Nature Neuroscience. 2001;4(12):1165.
[9] Lockley SW, Brainard GC, Czeisler CA. High sensitivity of the human circadian melatonin rhythm to resetting by short wavelength light. Journal of Clinical Endocrinology and Metabolism. 2003;88(9):4502-4505.
[10] Vandewalle G, Maquet P, Dijk DJ. Light as a modulator of cognitive brain function. Trends in Cognitive Sciences. 2009;13(10):429-438.
[11] Chang AM, Aeschbach D, Duffy JF, Czeisler CA. Evening use of light-emitting eReaders negatively affects sleep, circadian timing, and next-morning alertness. Proceedings of the National Academy of Sciences. 2015;112(4):1232-1237.
[12] Cajochen C, Frey S, Anders D, et al. Evening exposure to a light-emitting diodes (LED)-backlit computer screen affects circadian physiology and cognitive performance. Journal of Applied Physiology. 2011;110(5):1432-1438.
[13] Silvani MI, Werder R, Perret C. The influence of blue light on sleep, performance and wellbeing in young adults: A systematic review. Frontiers in Physiology. 2022;13:943108.
[14] Tosini G, Ferguson I, Tsubota K. Effects of blue light on the circadian system and eye physiology. Molecular Vision. 2016;22:61-72.
[15] O’Hagan JB, Khazova M, Price LL. Low-energy light bulbs, computers, tablets and the blue light hazard. Eye. 2016;30(2):230-233.
[16] Lee TM, Loh EW, Kuo TC, Tam KW, Lee HC, Wu D. Effects of ultraviolet and blue-light filtering on sleep: a meta-analysis of controlled trials and studies on cataract patients. Eye. 2021;35:1629-1636.
[17] Brøndsted AE, Sander B, Haargaard B, et al. The effect of cataract surgery on circadian photoentrainment: a randomized trial of blue-blocking versus neutral intraocular lenses. Ophthalmology. 2015;122:2115-2124.
[18] King A, Gottlieb E, Brooks DG, Murphy MP, Dunaief JL. Mitochondria-derived reactive oxygen species mediate blue light-induced death of retinal pigment epithelial cells. Photochemistry and Photobiology. 2004;79(5):470-475.
[19] Sparrow JR, Miller AS, Zhou J. Blue light-absorbing intraocular lens and retinal pigment epithelium protection in vitro. Journal of Cataract and Refractive Surgery. 2004;30(4):873-878.
[20] Zhao ZC, Zhou Y, Tan G, Li J. Research progress about the effect and prevention of blue light on eyes. International Journal of Ophthalmology. 2018;11(12):1999-2003.
[21] Lawrenson JG, Hull CC, Downie LE. The effect of blue-light blocking spectacle lenses on visual performance, macular health and the sleep-wake cycle: a systematic review of the literature. Ophthalmic and Physiological Optics. 2017;37:644-654.
[22] Singh S, Keller PR, Busija L, et al. Blue-light filtering spectacle lenses for visual performance, sleep, and macular health in adults. Cochrane Database of Systematic Reviews. 2023;8:CD013244.
[23] Shechter A, Quispe KA, Mizhquiri Barbecho JS, Slater C, Falzon L. Interventions to reduce short-wavelength (“blue”) light exposure at night and their effects on sleep: A systematic review and meta-analysis. Sleep Advances. 2020;1(1):zpaa002.
[24] Burkhart K, Phelps JR. Amber lenses to block blue light and improve sleep: a randomized trial. Chronobiology International. 2009;26(8):1602-1612.
[25] Turner PL, Mainster MA. Circadian photoreception: ageing and the eye’s important role in systemic health. British Journal of Ophthalmology. 2008;92:1439-1444.